Get your free demo
What are the benefits?
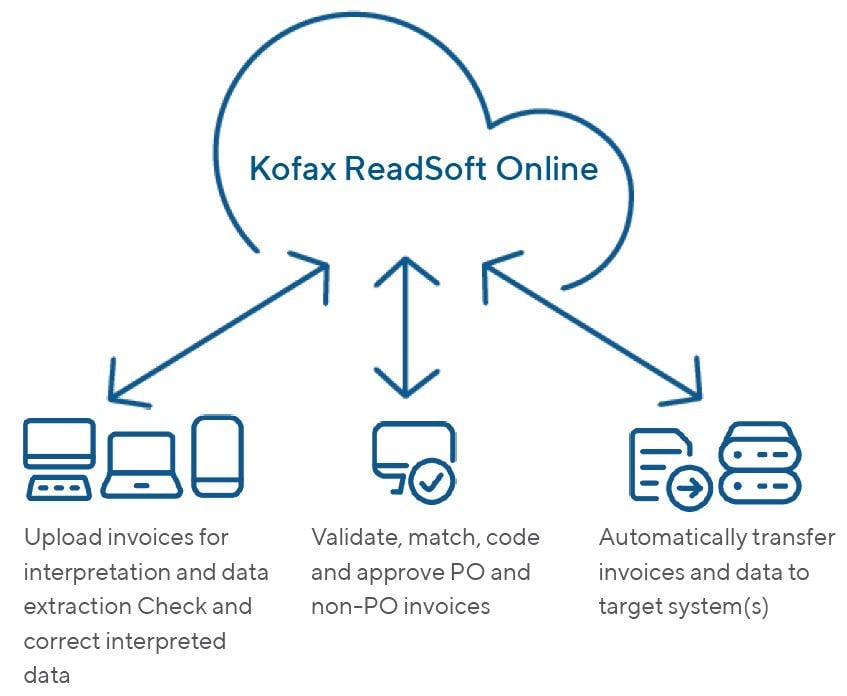
Process invoices seamlessly and affordably in the cloud:
- Oracle Financials Cloud
- Oracle NetSuite
- Microsoft Dynamics Navision (NAV)
- Microsoft Dynamics 365 – Finance and Operations (D365 F&O)
- Microsoft Dynamics 365 – Business Central (D365BC)
- Coupa Business Spend Management
Ready to get started with ReadSoft Online?
What is financial process automation (FPA)?
Financial Process Automation (FPA) solutions fully integrate with any ERP system to optimise the purchase-to-pay, order-to-cash and record-to-report cycles. Modernise and simplify your Accounts Payable and Sales Ordering processes with automation software, and you’ll be able to capture and extract information from any source, automatically routing it into an approval workflow, and transferring information into your system of record. FPA eliminates delays with error free processes, and provides total visibility into data.
By breaking financial process silos, organisations systematically increase efficiency and better working practices among staff, suppliers and customers, driving strategic business outcomes with complete process control and insights at their fingertips.
Purchase-to-Pay
Invoice automation is a natural first step towards process improvements for many organisations, but top performing organisations are 77% more likely to use a complete P2P solution. Automating the entire purchase-to-pay process, from purchase requisitions to payment approvals, offers opportunities for major gains in efficiency and cost savings.
Order-to-Cash
With around 86% of sales orders still received non-electronically, processes that incorporate manual tasks make order-to-cash efficiency and A+ customer service nearly impossible. Automating sales order processing, order fulfilment and payment advice processing reduces Days Sales Outstanding, accelerates handling of receivables, and gives staff and customers up-to-date information about payment status.
Record-to-Report
Automating financial postings and master data management ensures data accuracy, timeliness, and transparency so organisations can make better business decisions, have more satisfied customers and ensure regulatory and user compliance.
Book your demo, sign up for a free trial, or ask about Kofax ReadSoft Online pricing
Financial Process Automation from Twofold Ltd
Need to know more?
Accreditations & Partners